Plantar Fasciitis Treatment in Buffalo Grove & Chicago IL
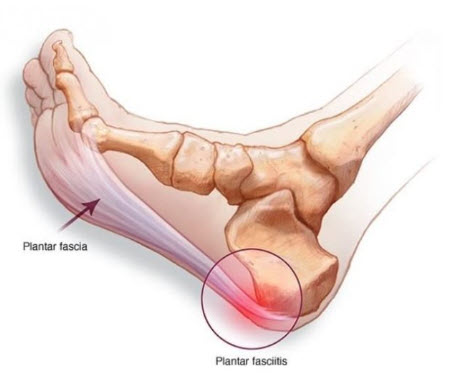
 Plantar fasciitis is a painful condition that occurs when the strong band of tissue that extends from the heel to the base of the toes becomes weakened where it attaches to the heel. This tissue is called the plantar fascia, and its primary purpose is to support the arch, so the foot remains flexible and resilient. The pain of plantar fasciitis is most intense in the morning or after other long periods of inactivity, becoming less intense as the plantar fascia “warms up” during activity. Commonly, plantar fasciitis is characterized by “pain on first steps in the morning”.
Plantar fasciitis is a painful condition that occurs when the strong band of tissue that extends from the heel to the base of the toes becomes weakened where it attaches to the heel. This tissue is called the plantar fascia, and its primary purpose is to support the arch, so the foot remains flexible and resilient. The pain of plantar fasciitis is most intense in the morning or after other long periods of inactivity, becoming less intense as the plantar fascia “warms up” during activity. Commonly, plantar fasciitis is characterized by “pain on first steps in the morning”.
What is Plantar Fasciitis?
Plantar fasciitis causes pain in the bottom of the heel. The plantar fascia is a thick, web-like ligament that connects your heel to the front of your foot. It acts as a shock absorber and supports the arch of your foot, helping you walk.
Plantar fasciitis is one of the most common orthopedic complaints. Your plantar fascia ligaments experience a lot of wear and tear in your daily life.
Too much pressure on your feet can damage or tear the ligaments. The plantar fascia becomes inflamed, and the inflammation causes heel pain and stiffness. Plantar fasciitis affects both sedentary and athletic people and is thought to result from chronic overload either from lifestyle or exercise
The cause of plantar fasciitis discomfort is still unclear. A study suggested that the condition may involve degeneration.
Plantar Fasciitis – One of the Most Common Causes of Heel Pain
One of the most common causes of heel pain is Plantar Fasciitis and has been estimated to affect over 2 million people in the US, resulting in more than one million visits to both primary care physicians and foot specialists. It involves inflammation of a thick band of tissue that runs across the bottom of your foot and connects your heel bone to your toes (plantar fascia).
Plantar fasciitis commonly causes stabbing pain that usually occurs with your first steps in the morning. As you get up and move, the pain normally decreases, but it might return after long periods of standing or when you stand up after sitting.
Plantar fasciitis is more common in runners. People who are overweight and those who wear shoes with inadequate support also have an increased risk of plantar fasciitis.
Main Symptoms of Plantar Fasciitis
 Plantar fasciitis typically causes a stabbing or throbbing pain in the bottom of your foot, near the heel. The pain is usually the worst with the first few steps after awakening, although it can also be triggered by long periods of standing or when you get up after sitting. The pain is usually worse after exercise, not during it.
Plantar fasciitis typically causes a stabbing or throbbing pain in the bottom of your foot, near the heel. The pain is usually the worst with the first few steps after awakening, although it can also be triggered by long periods of standing or when you get up after sitting. The pain is usually worse after exercise, not during it.
The major complaint of those with plantar fasciitis is pain at the bottom of the heel or sometimes at the bottom mid-foot area. It usually affects just one foot, but it can affect both feet.
Pain from plantar fasciitis develops gradually over time. The pain can be dull or sharp. Some people feel a burning or ache on the bottom of the foot extending outward from the heel.
The pain is usually worse in the morning when you take your first steps out of bed, or if you’ve been sitting or lying down for a while. Climbing stairs can be very difficult due to heel stiffness.
After prolonged activity, the pain can flare up due to increased irritation or inflammation. People with plantar fasciitis don’t usually feel pain during the activity, but rather just after stopping.
Main Causes of Plantar Fasciitis
Plantar fasciitis is common among people who are middle-aged and older. However, there are issues that can make the condition more common; including being obese or overweight, having high arches or flat feet, having a tight or short Achilles tendon (the tendon that connects the calf muscle to the heel), wearing shoes with poor or no arch support, and participating in certain sports like running.
Your plantar fascia is in the shape of a bowstring, supporting the arch of your foot and absorbing shock when you walk. If tension and stress on this bowstring become too great, small tears can occur in the fascia. Repeated stretching and tearing can irritate or inflame the fascia, although the cause remains unclear in many cases of plantar fasciitis.
Active men and women between the ages of 40 and 70 are at the highest risk for developing plantar fasciitis. It’s also slightly more common in women than men. Women who are pregnant often experience bouts of plantar fasciitis, particularly during late pregnancy.
You’re at a greater risk of developing plantar fasciitis if you’re overweight or obese. This is due to the increased pressure on your plantar fascia ligaments, especially if you have sudden weight gain.
If you’re a long-distance runner, you may be more likely to develop plantar fascia problems. You’re also at risk if you have a very active job that involves being on your feet often, such as working in a factory or being a restaurant server.
If you have structural foot problems, such as very high arches or very flat feet, you may develop plantar fasciitis. Tight Achilles tendons, which are the tendons attaching your calf muscles to your heels, may also result in plantar fascia pain. Simply wearing shoes with soft soles and poor arch support can also result in plantar fasciitis.
Plantar Fasciitis- The Health Risk Factors
Even though plantar fasciitis can develop without an obvious cause, some factors can increase your risk of developing this condition. They include:
- Age – Plantar fasciitis is most common between the ages of 40 and 60.
- Certain types of exercise – Activities that place a lot of stress on your heel and attached tissue — such as long-distance running, ballet dancing and aerobic dance — can contribute to the onset of plantar fasciitis.
- Obesity – Excess pounds put extra stress on your plantar fascia.
- Occupations that keep you on your feet – Factory workers, teachers and others who spend most of their work hours walking or standing on hard surfaces can damage the plantar fascia.
- Foot mechanics – Flat feet, a high arch, shortened Achilles tendon, or even an abnormal pattern of walking can affect the way weight is distributed when you’re standing and can put added stress on the plantar fascia.
- Extrinsic risk factors – Poor biomechanics or alignment
Complications & Medical Concerns, involving Plantar Fasciitis
Ignoring plantar fasciitis may result in chronic heel pain that hinders your regular activities. Changing the way you walk as a way to relieve plantar fasciitis pain might lead to foot, knee, hip or back problems.
Plantar Fasciitis Testing and Diagnosis
Your doctor will perform a physical exam to check for tenderness in your foot and the exact location of the pain. This is to make sure that the pain isn’t the result of a different foot problem.
During the evaluation, they may ask you to flex your foot while they push on the plantar fascia to see if the pain gets worse as you flex and better as you point your toe. They’ll also note if you have mild redness or swelling.
Your doctor will evaluate the strength of your muscles and the health of your nerves by checking your:
- reflexes
- muscle tone
- sense of touch and sight
- coordination
- balance
An X-ray or an MRI scan may be necessary to check that nothing else is causing your heel pain, such as a bone fracture.
Plantar Fasciitis Treatment
Plantar fasciitis is usually treated non-surgically with splints and exercises to help stretch the foot and Achilles tendon and to relieve inflammation, combined with custom orthotics designed to provide better support for the arch of the foot and the heel, and to relieve excess pressure on the heel. Orthotics are available for many different types of shoes, including dress shoes and athletic shoes.
Physical therapy is a key part of treatment for plantar fasciitis. It can help stretch your plantar fascia and Achilles tendons. A physical therapist can show you exercises to strengthen your lower leg muscles, helping to stabilize your walk and lessen the workload on your plantar fascia.
If pain continues and other methods aren’t working, your doctor may recommend extracorporeal shock wave therapy. In this therapy, sound waves bombard your heel to stimulate healing within the ligament.
AmnioFix® in the Treatment of Plantar Fasciitis
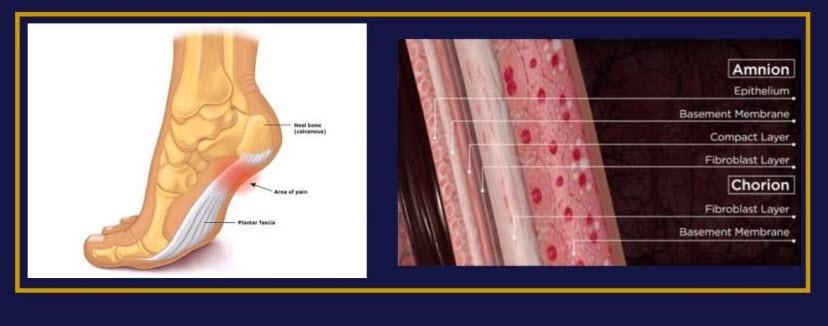
A study published in the journal Foot & Ankle International found that a single injection of AmnioFix® yielded “significant improvement” in plantar fasciitis symptoms and increased function.
Human amniotic membrane lines the innermost layer of placenta and amniotic cavity. AmnioFix® Injectable is a micronized dehydrated human amnion/chorion membrane allograft. AmnioFix may provide clinical benefit for soft tissue healing and inflammation reduction as well as provide an inflammation barrier.
Plantar Fasciitis Surgery / Surgeons
Surgery is the most dramatic therapy. This is done only in cases in which pain is severe or lasts more than 6 to 12 months. In a plantar fascia release, your surgeon partially detaches the plantar fascia from the heel bone. This reduces tension, but weakens the arch of the foot, and full function may be lost.
If you have a hard time flexing your feet even after consistent stretching, your doctor may recommend gastrocnemius recession. This surgery involves lengthening the calf muscle to increase ankle motion and release stress on the plantar fascia.
Surgery can result in chronic pain and nerve damage, so it should be considered only after trying other treatment options.
Most people don’t need surgery to relieve pain from plantar fasciitis. Instead, their condition improves through physical therapy, home treatments, and medical treatments. However, treatment can take several months to 2 years to improve your symptoms.
Plantar Fasciitis Exercises
Gentle stretches can help relieve and even prevent plantar fasciitis. Stretching your calves and the plantar fascia itself helps loosen your muscles and reduce heel pain.
It’s important to take time off from certain exercises, like running, to give the plantar fascia time to heal. Swimming and other low-impact activities can let you exercise without worsening your heel pain. When you start running again, be sure to begin slowly. Stop and stretch while exercising to keep the pain from returning. Remember to stretch before beginning your workouts, too.
Stretches for plantar fasciitis are easy to do. You’ll only need a few common props, like a chair and a foam roller or even just a frozen water bottle. Learn the right stretches to help heal and prevent plantar fasciitis.
How is plantar fasciitis diagnosed?
Diagnosis can usually be confirmed with an examination of the foot to look for areas of tenderness, mild swelling or redness, arch problems like flat or high arches, and stiffness or tightness in the bottom of the foot. Passive and active movements will be used to assess the pain and determine its source. X-rays may also be taken to rule out other potential causes of pain like a midfoot fracture or arthritis.
Chicago Custom Orthotics
Our custom orthotics help with the pain associated with plantar fasciitis by providing comfortable support for your feet. They are available for men’s dress shoes, women’s heels, sneakers, ice skates, skis, and athletic cleats. They are molded to your feet to treat your problem! An example of our custom orthotics can be found here.
When Experiencing Symptoms of Plantar Fasciitis – Request an Appointment at Global Podiatry, Today!